Retina Conditions
Age-related Macular Degeneration (AMD)
Age-related macular degeneration (AMD) is an eye disease that affects the sharp, central vision needed for activities like reading and driving. AMD is a leading cause of vision loss for people age 50 and older, and doesn’t cause complete blindness. There are 2 types: dry and wet. Dry AMD is more common, occurring as the macula gets thinner with age and progresses slowly over years. Wet AMD is less common but can cause faster vision loss due to abnormal blood vessel growth and damage the macula. Wet AMD is treatable with intraocular injections. There is no treatment currently for dry AMD. Where is the macula? The macula is located in the center of the retina, the light-sensitive tissue at the back of the eye. The retina instantly converts light, or an image, into electrical impulses. The retina then sends these impulses, or nerve signals, to the brain. Can I have both dry and wet AMD? Yes. All patients with AMD start out with dry AMD. Over the course of a lifetime about 10% to 20% of patients with dry AMD develop the wet form of the disease. It is important that you know that the changes of dry AMD may continue to progress even after you develop wet AMD. It is also important to understand that wet AMD always develops in a patient with previous dry AMD. So if you have the dry form and you notice new symptoms do not assume these new symptoms are due to progression of the dry changes. Let your doctor know so that he or she can determine if wet AMD has developed and if you need treatment. Treatment consists of intraocular antivegf injections. PDT laser is used in certain cases. Diabetic Retinopathy
Diabetic retinopathy is an eye condition that can cause vision loss and blindness in people who have diabetes. It affects blood vessels in the retina (the light-sensitive layer of tissue in the back of your eye). In some people with diabetic retinopathy, blood vessels may swell and leak fluid. In other people, abnormal new blood vessels grow on the surface of the retina. The retina is the light-sensitive tissue at the back of the eye. A healthy retina is necessary for good vision. If you have diabetic retinopathy, at first you may not notice changes to your vision. But over time, diabetic retinopathy can get worse and cause vision loss. Diabetic retinopathy usually affects both eyes. How does diabetic retinopathy cause vision loss? Blood vessels damaged from diabetic retinopathy can cause vision loss in two ways: 1. Fragile, abnormal blood vessels can develop and leak blood into the center of the eye, blurring vision. This is proliferative retinopathy and is the fourth and most advanced stage of the disease. 2. Fluid can leak into the center of the macula, the part of the eye where sharp, straight-ahead vision occurs. The fluid makes the macula swell, blurring vision. This condition is called macular edema. It can occur at any stage of diabetic retinopathy, although it is more likely to occur as the disease progresses. About half of the people with proliferative retinopathy also have macular edema. Anti-vegf injections, laser and surgery may be indicated to treat different stages of diabetic retinopathy. Retinal Detachment
Retinal detachment is an eye problem that happens when your retina (a light-sensitive layer of tissue in the back of your eye) is pulled away from its normal position at the back of your eye. In some cases there may be small areas of the retina that are torn. These areas, called retinal tears or retinal breaks, can lead to retinal detachment. What are the symptoms of retinal detachment? Not all patients with retinal detachment have the same symptoms. In fact, some patients have no warning signs at all. These are the warning signs: First, a sudden increase in the number or size of floaters in the vision is common. This may be accompanied by awareness of light flashes in the side vision. Finally, the sensation of a curtain or veil over part of the vision is usually alarming enough to get most people to call for an exam. It is important to recognize a retinal tear or detachment as promptly as possible because the problem may be easier to correct if caught in its early stages. If scleral buckling surgery, vitrectomy or a combination of vitrectomy with scleral buckle is required then surgery would be scheduled in a timely fashion. Retinal Vein Occlusions
Retinal vein occlusion is a blockage of the veins in the retina. There are two forms of retinal vein occlusion, both require treatment to prevent vision loss and other complications. Central retinal vein occlusion (CRVO) occurs when the main retinal vein is blocked, and may result in bleeding and swelling of the retina or macula, leading to a severe decrease in vision. Abnormal vessels may develop, and if they grow on the iris, a severe and a painful increase in eye pressure may develop. Branch retinal vein occlusion (BRVO) occurs when a branch of the main retinal vein becomes blocked, reducing blood flow to a portion of the retina, causing vision loss, although usually not as severe as in CRVO. Macular edema may develop with a BRVO as well. Retinal vein occlusion may be treated with intraocular injections and laser. Macular Pucker/Epiretinal Membrane
A macular pucker is scar tissue that has formed on the eye’s macula, located in the center of the light-sensitive tissue called the retina. The macula provides the sharp, central vision we need for reading, driving, and seeing fine detail. A macular pucker can cause blurred and distorted central vision. Macular Hole
A macular hole is a small break in the macula, located in the center of the eye’s light-sensitive tissue called the retina. The macula provides the sharp, central vision we need for reading, driving, and seeing fine detail. A macular hole can cause blurred and distorted central vision. Macular holes are related to aging and usually occur in people over age 60. Vitrectomy surgery is required most of the time to repair a macular hole. Central Serous Retinopathy (CSR)
Central serous retinopathy typically affects adults between the ages of 20 and 50. It appears as a small, round, swelling that develops underneath the retina that reduces or distorts vision. This is usually temporary. Vision generally recovers on its own within a few months without treatment. However if fluid persists treatment with PDT or "cold laser", focal laser, intraocular injection or systemic medications may be indicated. Vitreous Detachment
The vitreous is the gel-like fluid that fills your eye. It’s full of tiny fibers that attach to your retina (the light-sensitive layer of tissue at the back of the eye). As you get older, the fibers of your vitreous pull away from the retina. This is called vitreous detachment. It usually happens after age 50. If you notice symptoms that affect your vision, talk to your eye doctor. Floaters
Floaters are small dark shapes that float across your vision. They can look like spots, threads, squiggly lines, or even little cobwebs. Most people have floaters that don’t need treatment. But sometimes floaters can be a sign of a more serious eye condition. So if you notice new floaters that appear suddenly and don’t go away, speak to your eye doctor. Information provided courtesy of the US National Institutes of Health, National Eye Institute.
To learn more, please ask our doctors, or visit https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases |
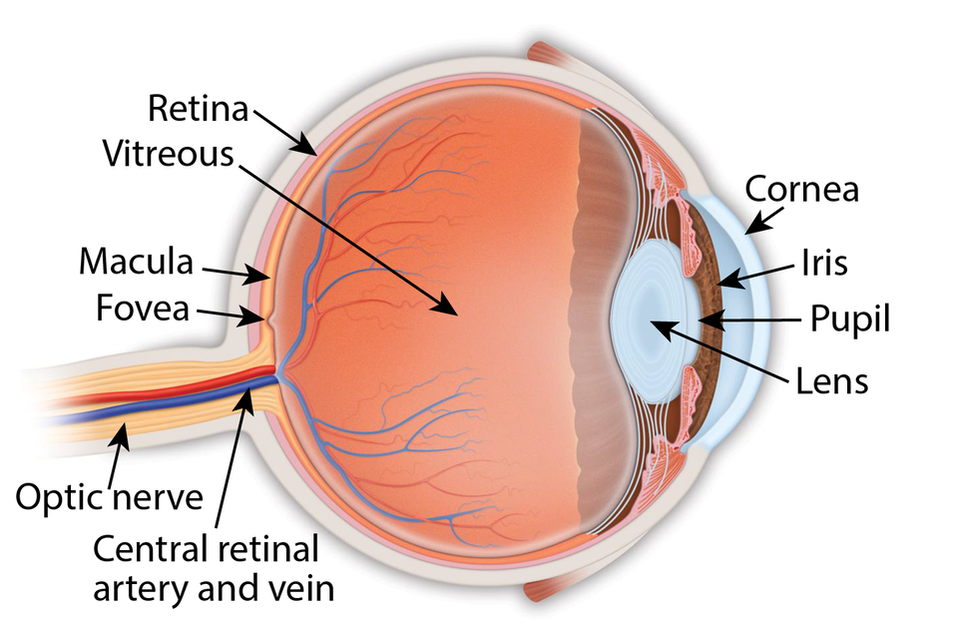
Eye Anatomy
Retina: the light-sensitive membrane in the back of the eye that converts light to electrical impulses that are sent to the brain through the optic nerve
Vitreous: also called vitreous humor, a thick, colorless gel that fills the large space in the middle of the eye, behind the lens Macula: the central retina that contains the fovea Fovea: a shallow pit in the center of the retina responsible for our sharpest straight ahead vision Optic nerve: carries the message of vision from the retina to the brain Cornea: transparent convex membrane that covers the pupil and iris of the eye Iris: colored part of the eye that consists of a muscular diaphragm surrounding the pupil and regulates the light entering the eye by expanding and contracting the pupil Pupil: dark circular opening at the center of the iris in the eye, where light enters the eye Lens: focuses light to produce an image on the light-sensitive cells of the retina. Nearly spherical and convex on both sides, it sits behind the pupil |
|
Copyright © 2021 Retina Consultants. All rights reserved.
|